Changes in your central vision can feel concerning, but you do not have to navigate them alone. At Retina Health Center, we combine advanced imaging with the expertise of seasoned retina specialists to help you regain confidence in your ocular health.
We specialize in macular hole treatment in Fort Myers and Naples, providing comprehensive care that includes state-of-the-art macular hole diagnosis, treatment, and surgery. Explore our process below, and when you’re ready to take the next step toward clarity, book your consultation today.
What is a Macular Hole?
A macular hole is a disorder in which the center portion of the retina, which is called the macula, develops a hole or a break. The macula is the portion of the retina that is responsible for a person’s ability to read fine print, to drive, and to do other detailed work.
When a hole develops in this area, it results in a reduction in one’s central vision, which can be mild to severe depending on how large the hole is and how long it has been present. Macular hole surgery is the best solution for treating this condition.
What Causes a Macular Hole?
Macular holes are most commonly seen in adults over the age of 60 and often develop without another major eye disease. In some cases, they may also be linked to conditions such as:
- high myopia (severe nearsightedness)
- macular pucker
- eye trauma
- diabetes
- retinal detachment
A macular hole usually affects only one eye, but in up to 15% of cases, the other eye may also develop the condition over time. As a result, timely macular hole treatment is needed under expert supervision.
Stages of Macular Holes
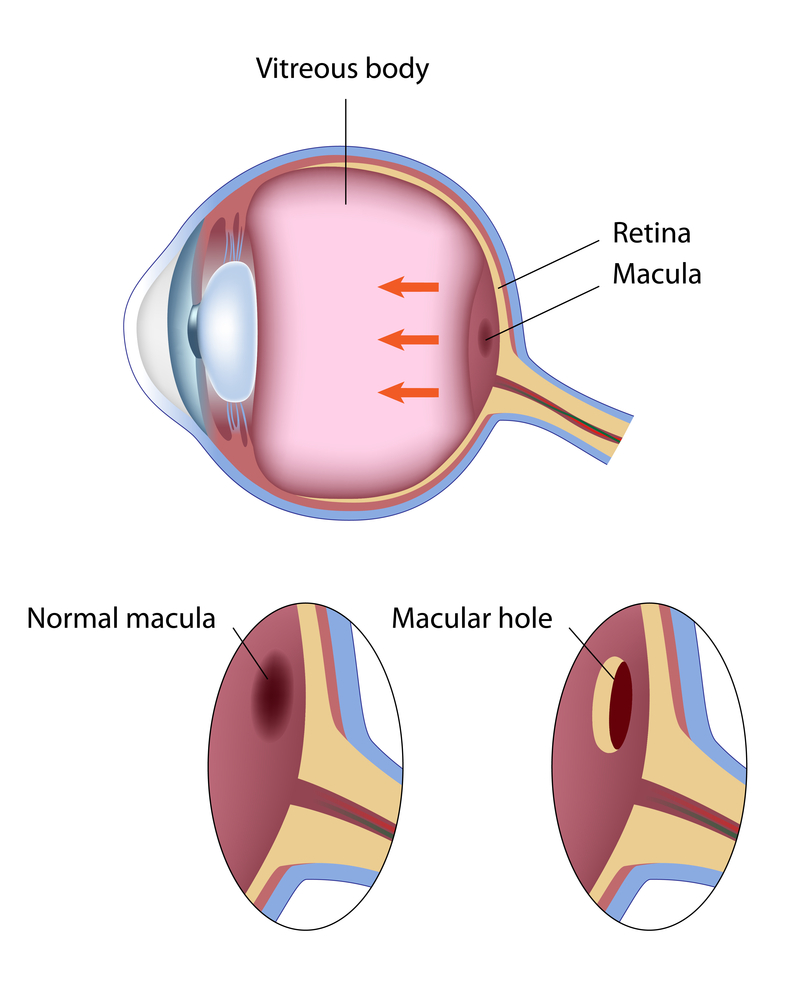
- Macular hole treatment varies depending on the four different stages of the condition. In early stages (stage 1 and 2) patients may notice only a slight distortion or haziness in their vision. Lines may look bent or crooked and in later stages (Stage 3 and 4) central vision is blurred and detailed vision can be lost.
- Macular holes can best be seen on a cross sectional image of the retina which can be obtained using Optical Coherence Tomography. A normal retina appears in image 1, whereas a macular hole can be seen in image 2.
- Macular holes are seen usually in people over age of 60 without any other eye diseases. However, macular holes can be associated to eye disorders such as nearsightedness (high myopia), macular pucker, trauma, diabetes and retinal detachments.
- Usually macular hole affects only one eye, but in up-to 15 percent of time the other eye maybe affected. Only a small percentage of stage 2, 3, and 4 macular holes can heal on their own; the majority will need eye macular hole surgery to improve vision. Surgery is often on an out-patient basis with local anesthesia. In general, once you have a stage 2, 3, or 4 macular hole, you are better off having surgery within four to six weeks. Typically, the longer you wait, the less likely you are to regain your vision after eye macular hole surgery. Visual recovery for macular holes that are over a year old tends to be less than those that are only a few weeks old.
How is a Macular Hole Diagnosed?
A macular hole is best diagnosed using Optical Coherence Tomography (OCT). This advanced imaging test provides a detailed cross-sectional view of the retina and helps eye care specialists assess the size and severity of the hole.
When is Macular Hole Surgery Needed?
Only a small percentage of stage 2, 3, and 4 macular holes close on their own. In most cases, macular hole surgery is recommended to improve the chance of preserving or restoring vision.
Timing matters. Once a stage 2, 3, or 4 macular hole is diagnosed, surgery is often recommended within four to six weeks. In general, the longer the surgery is delayed, the lower the chance of achieving the best possible visual improvement. Macular holes that have been present for over a year usually have a lower recovery potential than holes treated within a few weeks.
Macular Hole Surgery
Eye macular hole surgery involves removing the material in the center of the eye, called the vitreous gel. In most cases the tissue on the surface of the retina called the internal limiting membrane and other associated membranes are also removed. The gel is then replaced by a gas bubble. The gas bubble presses against the retina/macula and helps to close the macular hole.
Macular Hole Surgery Recovery
During surgery a gas bubble is typically used, which can last around 2 or 10 weeks depending on the type of gas used. Face down positioning is no longer required in all patients after surgery, but in some cases your physician may request this to improve the chance of success. When needed it is typically only for a few hours a day, and at night patients can usually sleep on their side. While the gas bubble is in your eye, you will be instructed not to fly as the bubble can expand and cause eye pressure elevation, glaucoma, pain and vision loss.
Recovery After Eye Macular Hole Surgery
Recovery after eye macular hole surgery depends on the type of gas used and the overall condition of the eye. The gas bubble may remain in the eye for about 2 to 10 weeks.
Face-down positioning is no longer required for every patient, but in some cases, your physician may recommend it for a few hours a day to improve healing. At night, many patients are allowed to sleep on their side.
While the gas bubble is still in the eye, flying is not allowed. Air travel can cause the bubble to expand, potentially leading to increased eye pressure, pain, glaucoma, and vision loss.
What to Expect After Surgery
Visual recovery can take time. Some patients notice gradual improvement as the eye heals and the gas bubble dissipates. Although a surgical macular hole treatment can improve central vision in many cases, the final visual result depends on factors such as:
- How long has the hole been present
- the size of the hole
- the stage of the condition
- overall retinal health
Early treatment usually offers the best chance for improvement.
What is Macular Pucker?
A Macular Pucker is a thin tissue that is similar to the skin of an onion or a piece of plastic wrap that has developed over the central portion of the retina, the macula.
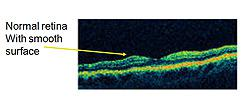
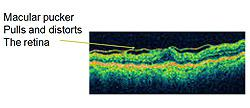
There are other names for this condition, including epiretinal membrane, wrinkled retina, pre-retinal fibrosis, or scar tissue. The condition can result in decreased vision and visual distortion. Straight lines can appear wavy. This is due to the tissue contracting, distorting, and thickening the retina. These changes can best be seen on a cross-sectional image of the retina, which can be obtained by the Retina Health Center specialists using Optical Coherence Tomography (OCT).
OCT delivers high-resolution images to help ophthalmologists determine whether a macular pucker is present. A normal retina appears in image 1, whereas a thickened and distorted retina due to a macular pucker can be seen in image 2. The distorted line at the top of the image represents a macular pucker. This condition is most common in patients over 50. Most of the time, it affects one eye.
However, it may affect the other eye later. Macular puckers are more common when other conditions are present, such as diabetes, inflammation, and trauma. Severe visual loss from macular pucker is rare; most patients notice blurred or distorted vision that is mild to moderate and progresses slowly. Most of the time, when symptoms are mild, macular hole treatment is not needed.
Personalized Retina Care Starts With One Conversation – Book Your Consultation Today!
If blurred or distorted vision is making reading or everyday tasks more difficult, surgery may be recommended to help improve how you see. The eye macular hole surgery typically involves a vitrectomy and careful removal of the scar tissue affecting the macula. While results vary from person to person, surgery often helps reduce distortion and improve vision, though it may not restore sight completely to normal.
At Retina Health Center, we carefully evaluate your symptoms, retinal health, and visual needs to determine whether surgery or another form of macular hole treatment is the right next step. A consultation with one of our specialists can help you better understand your options and move forward with confidence.
Frequently Asked Questions
Can I drive or work while the gas bubble is still in my eye?
Most patients must wait until the bubble shrinks significantly, as it severely distorts vision. Your specialist providing macular hole treatment will monitor your progress to clear you for safe driving.
Is it possible for a macular hole to recur after a successful surgery?
While recurrence is rare (under 5%), new traction or scar tissue can occasionally form. Routine follow-up imaging is essential to ensure the macula remains closed and your central vision stays stable long-term.
How do I know if my vision distortion is a macular hole or a cataract?
Cataracts typically cause overall cloudiness, whereas a macular hole creates a specific “dark spot” or “missing patch” in your direct line of sight. An OCT scan is the only way to confirm.
Are there any non-surgical alternatives, such as eye drops, to treat a macular hole?
Currently, no medications or drops can close a physical tear in the retina. Surgery remains the gold standard for macular hole treatment, physically repairing the tissue and preventing permanent loss.










